Information For Patients

Uterine cancer is the most common cancer of the female reproductive organs (www.gesund.bund.de).
It predominantly affects women after menopause; only about five percent are younger than 40. Until menopause, the lining (endometrium) of the uterus renews itself every month. Periodically, the upper layers are shed and expelled with menstruation. Changes to the uterus lining in which individual cells turn into cancer cells are more common during and after menopause.
In Western countries, uterine body cancer is twice as common as cervical cancer.
In Germany, Austria and Switzerland, almost 15,000 women are diagnosed with cancer of the uterine corpus (www.ecis.jrc.ec.europa.eu) every year.
A major risk factor is prolonged, elevated estrogen concentration in the female body. Women with menstrual irregularities, late menopause, childlessness, or certain hormone replacement therapies have an increased risk of developing this type of cancer.
Lifestyle diseases such as obesity, high blood pressure or type 2 diabetes mellitus can also increase the risk of tumors. It is known that obesity increases estrogen production. Whether there is a risk from phytoestrogens (estrogen-like substances in foods) has not yet been clarified. However, hormone therapy with estrogen alone certainly increases the risk (www.gesund.bund.de).
Cancer at an early stage is rarely detected during routine examinations. However, the disease becomes apparent relatively early with sudden, abnormal bleeding. Post-menopausal bleeding, irregular bleeding and flesh-colored discharge are in principle always suspicious and should be examined.
Abnormal uterine bleeding during or after menopause may be an indication of uterine cancer.
First, your gynecologist will ask you about your general health (medical history) and perform a gynecological exam. A sonography probe is then inserted into the vagina to assess the lining of the uterus (endometrium).
If the endometrium is conspicuously thickened, then the suspicion of cancer of the uterine body is studied by means of endoscopy (hysteroscopy) and abrasion (also called “curettage”). These surgical procedures are relatively complex, are performed under general anesthesia, and carry the risk of bleeding, infection, or other complications of surgical procedures, such as injury or perforation of the uterus or even anesthetic incidents.
The doctor uses a miniature camera to look inside the uterus. It will check whether any conspicuous changes in the endometrium are visible. Following hysteroscopy, the superficial portion of the endometrium is being removed. Following hysteroscopy, a biopsy of the uterus lining is taken and sent to the laboratory for examination. The biopsy may be taken from an area of the uterus lining that has the characteristics of cancer (targeted biopsy) or be scraped from the top layer of the womb lining (curettage).
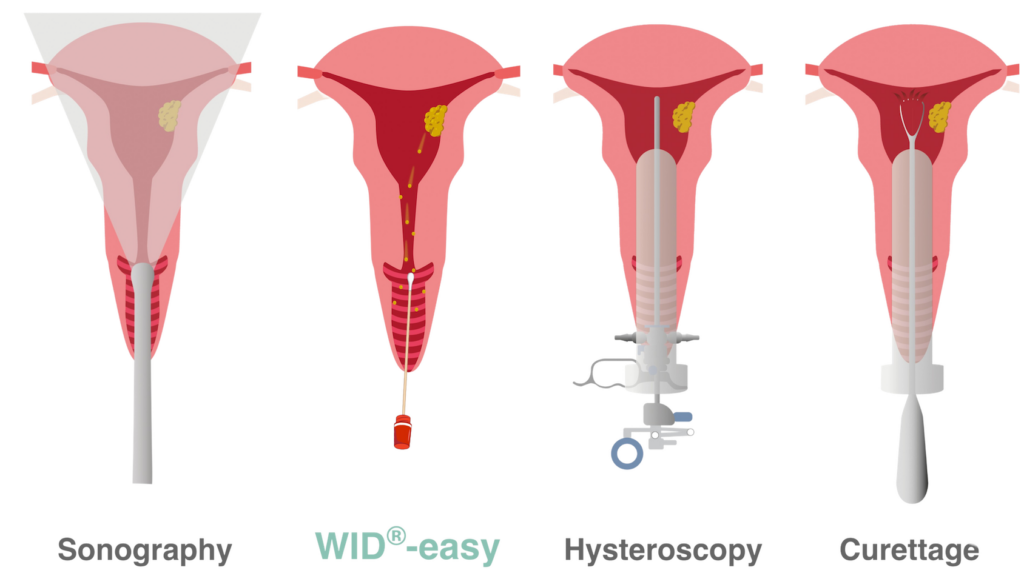
During hysteroscopy and curettage, the cervix is surgically dilated to allow instruments to be inserted into the uterine cavity. With the WID®-easy test, on the other hand, a swab from the upper vaginal area is sufficient.
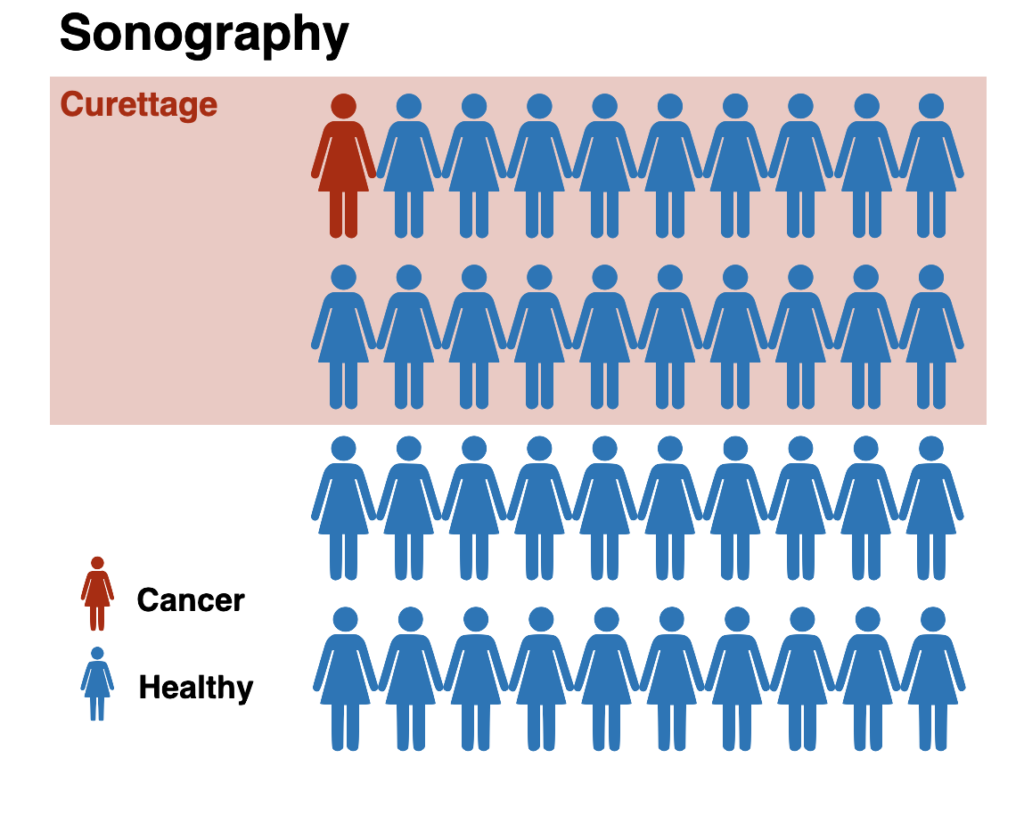
Out of 40 women who suffer from abnormal bleeding during or after menopause, about one woman will have uterine cancer. Nevertheless, the sonography will sound the alarm in 20 of these women (reddish background), and the women have to undergo curettage. Of these 20 women, 19 women do not have cancer.

In the same situation, the WID®-easy test will only have a positive result in two women, so that only two women will have to undergo a curettage (highlighted in red). Of these two women, only one does not have cancer.
Compared to transvaginal sonography, significantly fewer women who do not have cancer receive a false positive test result (“false alarm”) with the WID®-easy test. As a result, significantly fewer curettages need to be performed. With sonography, there are twenty women, and with the WID®-easy test, there are only 2 women who need a curettage. That’s a 90% reduction.
In a direct comparison between the WID®-easy test and the ultrasound method, it was shown that with the WID®-easy test there is only one woman without cancer for every woman with cancer who has to undergo a scraping (positive predictive value [PPV] of 50%), while with ultrasound there are 19 women for every woman with cancer who have a scraping, even though it later turns out that they do not have cancer (positive predictive value [PPV] of 5%). Thus, the WID®-easy test reduces the number of necessary surgical interventions in women who do not have cancer by as much as 95%.
(Source: Evans et al., The Lancet Oncology, 2023)
The test is very simple to perform: your doctor will take a swab from your vagina, very similar to the swab that is taken during your cervical cancer screening (“PAP smear”).
The sample is analyzed in the laboratory using PCR (similar to a Covid test) and the result is communicated to your doctor, who will discuss the result with you.
(Quelle: www.eutops.institute)
The WID?-easy test is arranged through your doctor. They will collect the sample and make sure it is sent for testing. Once your results are ready, your doctor will explain them to you clearly and discuss what they mean and whether any follow-up is needed.
If you would like to have the WID?-easy test, please speak with your doctor. They can help you decide if the test is right for you.
You can also call 087 148 9309 or email customer_care@ngms.co.za to get a list of doctors and facilities that already offer the WID?-easy test.

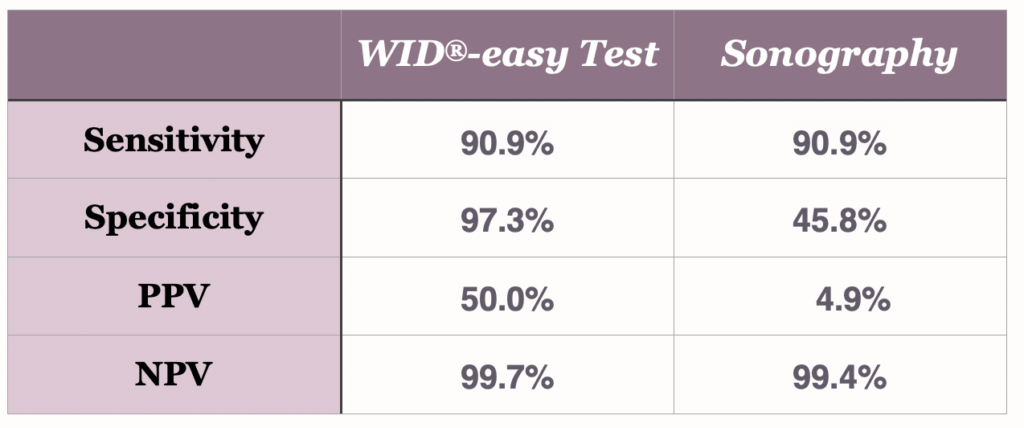
The WID®-easy test is characterized by extremely high values for sensitivity (90.9%), specificity (97.3%) and negative predictive value (99.7%).
Vor allem aber ist der positive Vorhersagewert mit 50 % zehnmal höher als der der Sonographie, deren PPV nur 5 % beträgt (Evans et al., The Lancet Oncology, 2023).
The WID®-easy test is a so-called epigenetic DNA methylation test.
DNA” is the term used to describe the human genetic material that parents pass on to their children. It consists of various long filaments (“chromosomes”) that are tightly coiled in every cell of the body. DNA plays an important role in controlling biological processes of the cell. Different regions on the DNA have different functions.
The so-called “DNA methylation” is a process that controls the activity of the different DNA regions. You can think of methylation as little marks on DNA.
This makes it possible for different processes to take place in different cells and for the cells to take on different tasks. DNA methylation is therefore not a genetic mutation, but merely a modification of the DNA.
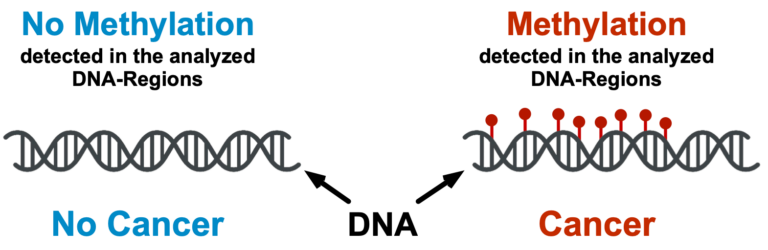
The WID®-easy test measures the methylation status of DNA regions known to be differentially methylated in uterine cancer.
Environmental influence on genes
Unlike the static DNA sequence, epigenetic DNA methylation patterns are subject to change and can also be influenced by the environment and personal lifestyle.
Providing Quality & Effective Solutions To The Research & Diagnostic Industry. Established in 2017, NextGen Molecular Supplies is South Africa leading suppliers of products and services to the biological research, diagnostics, and point of care market.
© 2026 NextGen Molecular Supplies.
Visit:
12 Clamart Road
Richmond
2092
Johannesburg
South Africa
Call: +27 87 148 9309
Email: customer_care@
ngms.co.za